Diabetes mellitus (DM) is a disease of epidemic proportions with a projected increase in worldwide prevalence from 360 million in 2011 to 552 million by 2030. Asia harbours 60% of the global DM population (4.7 billion), with the highest prevalence in Southeast Asia.
In Singapore, the number of adults with diabetes is projected to increase from 440,000 to 1 million in less than 30 years. The declaration of war against diabetes is timely as the projected number of diabetes in the different ethnic groups will vary. By 2050, 50% of the Malay and Indian population in males aged 60-69 years old being afflicted the most, followed by 30% in the Chinese population.
Cardiovascular diseases (CVD) account for more than half the mortality and morbidity among patients with diabetes. CVD complications of diabetes lead to disability, reduced quality of life, and hospitalisations, resulting in tremendous health economic impact. Southeast Asia has the highest rate of diabetes and Singapore has the highest risk of diabetic limb amputations in the world. Treating individuals with diabetes and CVD is 112% higher in cost than treating diabetics without complications.
A recent research at the National Heart Centre Singapore (NHCS) has discovered a unique lean diabetes pattern among Asian patients with heart failure (HF). These individuals develop diabetes despite a low body mass index (BMI), strikingly different from the conventional obesity-induced diabetes among Caucasians. These landmark findings were recognised for its importance and published in several high impact scientific journals (Tromp 2018 PLOS Med; Chandramouli 2019 PLOS Med).
A unique lean diabetic phentotype in Asians
Conventionally, diabetes is attributed to obesity, defined by BMI, resulting in hyperinsulinemia, glucose intolerance and insulin resistance. Beyond this classical paradigm and other well-defined diabetic conditions (Type 1 diabetes, maturity onset diabetes of the young, gestational diabetes), the lean diabetic phenotype has emerged as an interesting conundrum. The World Health Organisation (WHO)’s recommended cut-offs for normal and underweight categories among Asians are BMI 18.5–22.9 kg/m2 and <18kg/ m2, respectively. The prevalence of diabetes among Asians who fall within this normal or underweight range (BMI<23kg/m2) is increasingly high. Lean diabetes among asymptomatic Asians has been previously established and well-characterised by the absence of ketosis on withdrawal of insulin, a relatively early age of onset and associated with malnutrition and poor socioeconomic status. The WHO previously distinguished malnutrition-related diabetes from Type 1 and Type 2 diabetes in their former guidelines, however, it was removed in the later iterations due to insufficient evidence for causality. There is growing body of literature on this tropical diabetic phenotype that urges reconsideration.
Lean diabetes among Asian patients with heart failure
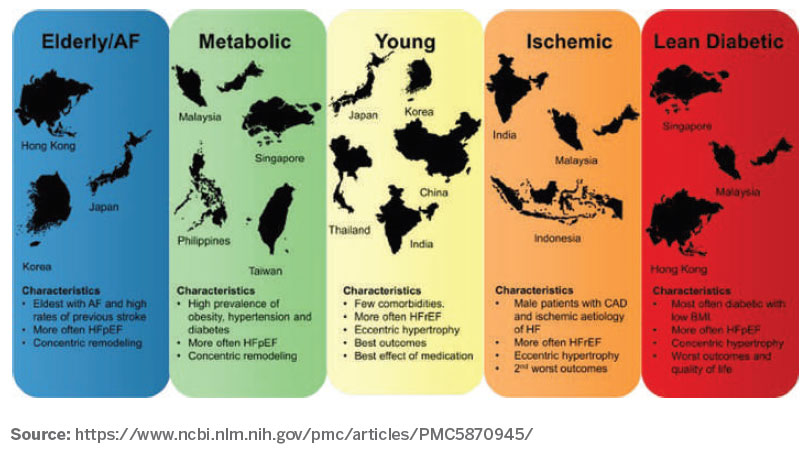
Professor Carolyn Lam, Clinician Scientist and Senior Consultant from Department of Cardiology, NHCS and her research team at NHCS demonstrated for the first time that lean diabetic phenotype also exists among patients with HF in Asia and that these patients have the worst outcomes. Dr Jasper Tromp, Research Fellow, NHCS, and fellow colleagues utilised the Asian Sudden Cardiac Death in Heart Failure (ASIAN-HF) Registry to analyse 6,480 patients with chronic HF from through latent class analysis. Interestingly, comorbidities naturally clustered into five distinct groups, namely, the elderly/ atrial fibrillation, metabolic, young, ischaemic and lean diabetic clusters. Among these comorbidity clusters of HF, the lean diabetic group with low BMI (<23 kg/m2) was associated with a predominance of HF with preserved ejection fraction (HFpEF), more concentric left ventricular enlargement, worst quality of life, more severe symptoms of HF and highest rate of mortality and morbidity outcomes. A prominence of the lean diabetes group in Southeast Asia, particularly Singapore, Malaysia and Hong Kong, was also evident. This article was published in PLOS Medicine in March 2018.
Visceral and epicardial fat: Potential culprits in lean diabetic heart failureThe research team has shed more light into this unique phenotype by identifying a possible detrimental role for ‘lean-fat’ among lean diabetic patients with HF. For the same given BMI, a higher percentage body fat is noted among Asians, compared to Caucasians. They recently reported that among individuals with HF (from ASIAN-HF Registry), those who were lean-fat (low BMI, high abdominal fat) were more likely to be women, from low-income countries in South/Southeast Asia, have high prevalence of diabetes, worst quality of life and worst HF outcomes, compared to their muscular counterparts in the obese-thin group (high BMI, low abdominal fat). Another interesting finding was that women with HF were also found likely to have diabetes at a lower BMI compared to men (≥23 vs. ≥27.5 kg/ m2). They have demonstrated that adding simple abdominal measure (waist-to-height ratio) to BMI in clinics has stronger prognostic ability among patients with HF than using BMI as a standalone marker. Together, these data suggested that visceral obesity could play a central role in cardiac pathology of lean diabetes. In low-middle income countries, foetal undernutrition, maternal insufficiency, the ‘thrifty gene’ hypothesis and predisposition towards visceral fat deposition are chiefly implicated in lean diabetes. Specifically, epicardial fat, the local visceral fat surrounding the heart, is particularly detrimental. This article was published in PLOS Medicine in September 2019. While there are no effective therapeutic options available to-date for this vulnerable group of individuals with lean diabetes and HF, particularly so for those with HFpEF, the research team is currently exploring prevention of CVD onset through early identification of high-risk diabetic individuals and the possibility of management through aggressive preventive therapy. 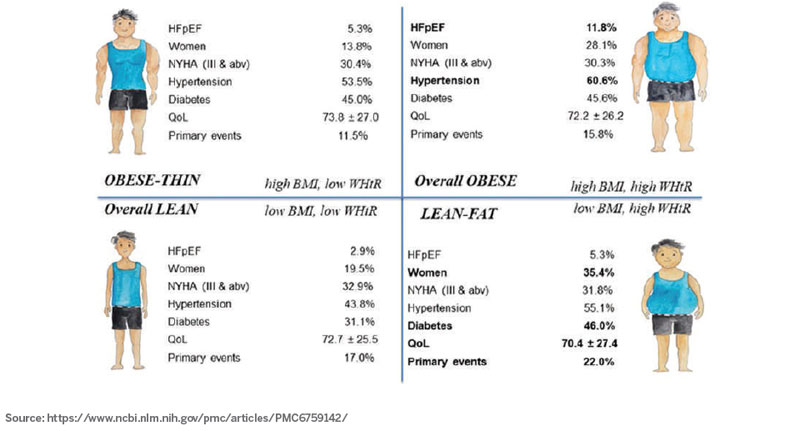
|
Tags:
;
;
;
;
Internal;
;
SingHealth;National Heart Centre Singapore;
Article;
Murmurs (NHCS);Tomorrow's Medicine;
;
;
;
;
Tomorrow's Medicine;Research
This article was first published in NHCS' newsletter Murmurs Issue 36.
